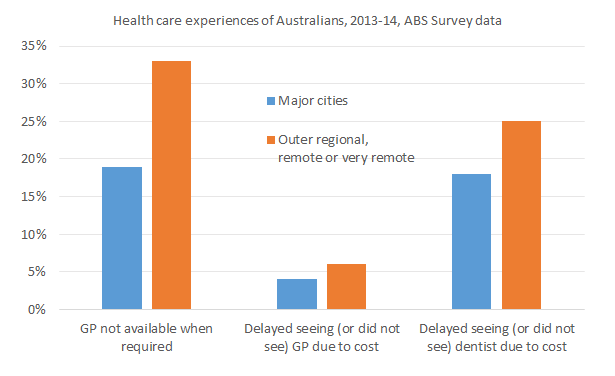
 There are large differences in access to health care between Australians living in major cities and those living in regional and remote areas, as confirmed by 2013-14 ABS survey data on patient experiences published last Friday (see chart above). Of course, some differences are to be expected, as it would be very costly to ensure the same level of medical services across the whole country, but it’s likely there are cost-effective measures that can be taken to improve health care in regional and remote areas.
There are large differences in access to health care between Australians living in major cities and those living in regional and remote areas, as confirmed by 2013-14 ABS survey data on patient experiences published last Friday (see chart above). Of course, some differences are to be expected, as it would be very costly to ensure the same level of medical services across the whole country, but it’s likely there are cost-effective measures that can be taken to improve health care in regional and remote areas.
At an Economic Society of Australia Queensland branch seminar earlier this month, Dr Abby Kamalakanthan of Grant Thornton spoke about the economics of regional and remote service delivery. In her talk, Abby referred to a nice paper from Grant Thornton on rural and remote health care, Making it work: Sustainable solutions for rural and remote primary healthcare. The paper notes (on p. 3):
Medicare funding is needed to make the employment of NPs [Nurse Practitioners] and PAs [Physician Assistants] worthwhile, to enable them to provide after hours care, and to reduce GP resistance to alternative types of primary health care professionals.
It appears that the Australian Medical Association (AMA) has been resistant to physician assistants, in particular, claiming they take clinical placements away from trainee doctors (see Turf war over physician assistants). This may be the case, but would suggest a need to fund more training positions in hospitals, rather than for abandoning the physician assistant concept, which appears one way of delivering cost-effective health care to regional and remote Australians. Perhaps the GP co-payment (if it actually goes ahead) could be used to fund more training positions for doctors and physician assistants, and for expanding Medicare coverage for work undertaken by nurse practitioners and physician assistants? This would probably be a better use of the money than the massive $20 billion medical research fund that was proposed by the Government.
